In a webinar sponsored by flipMD, from GoodRx, panelists discussed how the company is helping healthcare businesses optimize product development, marketing and go-to-market strategy, user adoption and more – all through collaboration with practicing physicians.
Panelist Dr. Gregory Hanson, co-founder of flipMD, shared how he developed the idea for flipMD when he and his wife lived in South Philadelphia during his residency when he was moonlighting as a consultant to make ends meet. That’s when he became aware of the lack of a platform specific to physicians to work with healthcare innovation companies looking for medical expertise.
“The idea for flipMD really came about from figuring out that it was a pretty big challenge for companies to find specific physicians, whether a practicing neurosurgeon to a nephrologist. It was just to make it easier for companies to be able to work with any type of physician from residents and fellows through early mid-career, late stage attending physicians or even retired physicians. That was the initial impetus and that’s why we built the company.”
The Covid-19 pandemic – coupled with ongoing healthcare industry challenges such as staff resources, hospital consolidation, and moral injury – has prompted a trend in physicians seeking alternate career solutions. At the same time, healthcare startup and growth stage companies oftentimes look to engage medical talent to provide useful insights to maximize and validate their work. Together, companies and physicians can mutually benefit each other: companies can hire physicians who possess the right expertise for their project, while physicians have the flexibility to pursue new opportunities outside of their clinical work.
Emergency Medicine physician, Dr. Caitlin McCord Delaney, assistant professor of Clinical Emergency Medicine with Georgetown University, described this demand for a fuller career from physicians and explained that they are also motivated by wanting to share their perspective on what’s working and what’s not in the health system.
“I’ve really seen a huge uptick in people’s interests in health tech and in new products and in, ‘What can we do to actually fix our healthcare system?’ There’s a huge demand right now from physicians who are looking for these different types of roles, they’re wanting to learn more about what’s out there,” Delaney said. “One of the things that I think is really significant about a platform like [flipMD] is that it allows you to cross-pollinate those different sectors. It’s good to have people who know something about both sides of it and to have the ability to work with those who have that different perspective.”
Another facet of the webinar discussion was the job of helping healthcare entrepreneurs find a suitable physician match for their needs. Dr. Jonathan Larson, president of Hey Doctor with GoodRx Care Provider Network, said it can be a monumental effort for companies to perform that task on their own.
“It’s great to connect to physicians, but we’re not all made alike. Our training and education and experiences are diverse. And so really finding that right fit so you don’t spend a bunch of money on somebody that maybe can talk a good game, but when it comes to bringing substantive information that really helps you move forward, they may just not be the right fit.”
And not finding the right fit can be costly. Among some of the interesting facts discussed was that the marketing budget for seven of the 10 largest pharmaceutical companies eclipses their R&D spend many times over. Moreover, in the medtech industry, the average cost to bring a product from concept to market is $31 million.
“Every company is addressing a need in healthcare and trying to create a solution that will be adopted by the majority, but it’s led to a very crowded marketplace. And so, it’s most important that we spend time thinking about how to differentiate and stand out in this market,” noted Lauren Hanson, founder and Head of Product with flipMD from GoodRx and the webinar moderator. “At the end of the day, if patients and physicians aren’t using your product, then even if it’s the best, you’re not making that big of an impact.”
To download and watch the webinar to learn more about how flipMD is working with healthcare companies to help match them with clinician expertise, please fill out the form below.
Uncategorized
OVID-19 continues to haunt some patients, with many suffering from so-called long COVID. Women and those with high body mass index (BMI) may be at higher risk for the condition, a new study has found.For their study, published Wednesday on PLOS Global Public Health, a team of researchers conducted a survey to “characterize the burden and predictors” for long COVID.Long COVID, also known as post-COVID syndrome, is the condition wherein the symptoms patients develop during or after a COVID-19 infection persist for over 12 weeks after being diagnosed with it. Symptoms may range from coughing, fatigue and breathlessness to brain fog, tinnitus and chest pain.”Ongoing symptomatic COVID-19 or post-COVID-19 syndrome is estimated to be adversely affecting the day-to-day activities of 836,000 people in the United Kingdom according to the ONS (Office for National Statistics, UK) report, with 244,000 saying their ability to undertake day-to-day activities had been ‘limited a lot,'” the researchers wrote.
To shed further light on the condition and potentially inform healthcare services, the researchers surveyed people in Norfolk, East England U.K. who were diagnosed with COVID-19 in 2020. In total, some 1,487 people participated in the survey, wherein they answered queries about pre- and post-COVID conditions such as breathlessness, loss of taste or smell, and their use of healthcare services related to long COVID.”We wanted to find out what factors might make people more or less susceptible to developing long COVID,” one of the study authors, Vassilios Vassiliou of the University of East Anglia’s (UEA) Norwich Medical School, said in the university’s news release.Of all the participants, 774, or 52.1% experienced long COVID. What’s interesting, however, is that more women had the symptoms compared to men, with the male sex appearing to be “protective of post-COVID symptoms” compared to the female sex.Having a higher BMI was also associated with higher risks of developing long COVID.”It was found that female sex and high BMI are associated with higher likelihood of developing post-COVID19 syndrome,” the researchers wrote. “Those two factors have a significant predictive value in the use of further health services among those diagnosed with post-COVID19 syndrome.”The results, they say, are in line with another previous research in England, wherein females were also found to have higher long COVID rates than males.This sheds further light on the condition that many continue to suffer from. According to the U.S. Centers for Disease Control and Prevention (CDC), for instance, long COVID has also been more often observed in some people such as those who had severe COVID-19, while those who weren’t vaccinated for COVID-19 may also face higher risks for it.The impact of long COVID may go beyond just the patients, too, as an expert pointed out that it may also have a $3.7 trillion impact on the U.S. economy. Hence, the results of this study provide valuable information about long COVID and the people who are most likely to suffer from it.”We hope that our work will help policymakers plan local services and also inform the wider public of the scale of the long COVID pandemic,” Vassiliou said, as per UEA.”Our academic colleagues at the University of East Anglia have really helped local health and care organizations to identify local patients at risk of long COVID, helping us to do all we can to support them on their recovery journey,” another study author, Mark Lim, added.
An insightful study analyzing what contributes to the sharpness of mind in old age has found evolutionary hints.The study, which was published in the peer-reviewed Chinese journal Science Bulletin, found that more developed frontal lobes were associated with sharp minds in some old people. The reason behind this occurrence may be attributed to natural selection in human evolution.“Our team initiated the Beijing Ageing Brain Rejuvenation Initiative in 2008, which focused on elderly people with cognitive impairment because they needed more attention. But during our community-based research, we found there was a group of elderly people who aged more slowly and had a higher quality of life,” Chen Yaojing, study corresponding author and a researcher at Beijing Normal University, said, reported South China Morning Post. “We want to learn from them and find out ways to keep our brain in a healthier state.”It was found during the study that people who had successful cognitive aging (SCA) had a better preserved frontal region of the brain. Meanwhile, people with mild cognitive impairment (MCI) exhibited structural deterioration in the temporal region of the brain.
The authors put forward a “frontal preservation, temporal impairment (FPTI)” hypothesis to provide an explanation for the differences in individuals’ cognitive aging.The frontal lobes are associated with cognitive functions, such as decision-making, problem-solving, and attention. Interestingly, the frontal lobes are one of the main features that separate human beings and animals. The frontal lobes are proportionally larger in humans than in other species of animals.Chen said the human frontal lobe was the most recent one to evolve and it exhibited age-related decline faster than other abilities.“There’s a theory called ‘last in, first out’. The newest part in evolution will decline first because human beings tend to save their survival abilities to the end,” Chen said. “So, for most elderly people, the functions of their frontal lobes decline early. But for people with successful cognitive aging, their frontal lobes are preserved well.”The temporal lobes are responsible for processing auditory information and preserving memory. Structural abnormalities in this region have been associated with pathological cognitive aging, according to researchers.Three groups of older adults aged between 70 and 88 were recruited for the study. These included 64 successful cognitive aging individuals, 68 mild cognitive impairment patients, and 66 cognitively normal controls.For the study, Chen and her colleagues analyzed gray matter volume, gray matter networks, and white matter network characteristics of the three groups.Compared to the other two groups, the SCA group performed better on all three parameters.“If our hypothesis is proven true, in the future we can develop the frontal lobes or slow the aging of temporal lobes,” Chen concluded. “This is a multidisciplinary effort.”
Patient privacy is evolving rapidly in the post-Dobbs era, healthcare and life science lawyers said in a webinar hosted by the American Bar Association on Wednesday.
“For now, a request from law enforcement personnel for protected health information is not valid unless it is pursuant to a process or as otherwise required by law,” said Lynn Barrett, a healthcare lawyer at Wachler & Associates.
Barrett and other panelists discussed what the Health Insurance Portability and Accountability Act (HIPAA) actually protects as it pertains to reproductive health data following the Dobbs decision in June and how the Office for Civil Rights (OCR) is carrying out those rules. Physicians, reproductive clinics and femtech companies need to understand this intimately to mitigate liability as well as protect patients.
Barrett, who is based in Florida where abortion is restricted, explained that if a patient were to go to their doctor and say they’re pregnant but don’t plan to have the baby, the provider wouldn’t be required to disclose that information to a law enforcement officer.
“What OCR is saying is that the intention to do something cannot be reported under HIPAA,” Barrett said.
The OCR worked with the American Medical Association and other medical organizations to develop their legal position, which is, “It would be inconsistent with professional and ethical standards to disclose to law enforcement anything regarding an individual’s interest, intent or prior experience with reproductive health,” Barrett said.
An interesting situation will be the federal preemption issues that occur if a physician in Texas or Florida or another restrictive state decides to call law enforcement, Barrett said, referring to when federal law and state law conflict each other.
When it comes to medical information that’s not shared with a provider, but that’s related to a personal device, such as a cellphone or laptop, it’s even trickier. HIPAA does not protect information on personal devices.
“If law enforcement suspects that an individual has had an illegal abortion, they could go and request access to that individual’s phone, their applications that they‘re using, their femtech apps, anything like that,” said Bethany Corbin, a femtech lawyer at Nixon Gwilt Law.
As a result of increased privacy concerns, some femtech apps, such as the period tracking app Flo, have enabled an “anonymous” mode, Corbin said. Still, she cautioned against users having a “false sense of security” because it’s unclear what “anonymous” means.
“That’s something we’re going to have to continue to watch to see how many apps come out with those modes, and if there’s any further regulation of that,” Corbin said.
The value of health data on the black market, just a general healthcare record is about $250, Corbin said. And if you compare that to something like a credit card, a credit card goes for about $5.60 on the black market. So the value of health data is already hugely increased from almost any other type of data you can get on the black market, Corbin said.
Some femtech companies have added a paid version of their free apps which adds more privacy, so customers can have a sense of security, but this is also new territory and there needs to be more regulation, Corbin added.
Another panelist, Heather Deixler, a partner at Latham and Watkins in the healthcare and life sciences practice area, said there’s a high need for a federal privacy law to protect reproductive healthcare information because the “patchwork” laws that vary state by state are very difficult to navigate.
Deixler said there’s an analogy to draw between how patient data is protected when it involves reproductive health and when it involves substance use disorder. For example, she said, when a patient is recovering from substance use disorder, their patient information is protected from law enforcement, even though what they’re doing is engaging in illegal acts of abusing substances.
“Taking that approach could be a really good way to limit this [reproductive health] information from being disclosed to law enforcement,” Deixler said.
Deixler also described how the Federal Trade Commission has reacted to privacy concerns. In one case she described, the FTC sued data broker Kochava for selling patient data that tracked when people visited a reproductive health clinic.
In another case, the FTC sued period tracking app Flo for selling data to Facebook and Google without the patient’s consent.
“They were saying they weren’t sharing data with third parties but they were,” Deixler said of Flo. “Part of what the FTC did was enforce transparency and said you need to get consent with individuals before sharing information.”
The case was a “wake up call” for people using these apps, Deixler said.
In a segment on what tech companies should be doing amid privacy issues, Deixler suggested tech companies use end-to-end encryption to protect patient data, limit the collection and sale of information that can reveal pregnancy status, stop using artificial intelligence tools that reveal pregnancy status, and vet data sharing relationships.
Photo: JuSun, Getty Images
Medical device manufacturer iCAD is integrating Google Health’s mammography AI technology into its suite of breast imaging AI products, the Nashua, N.H.-based company announced Monday.
The two companies are entering into a development and commercialization agreement. In fact, the agreement marks Google’s first commercial partnership to deploy its breast imaging AI model into clinical practice.
“By combining the two high performing technologies, we get a superior algorithm that can detect more cancer, reduce false positives and speed reading time,” iCAD CEO Stacey Stevens said in an interview.
Under the partnership, iCAD will validate Google’s mammography AI model and eventually incorporate it into its products for clinical use. The company said it will integrate the tech into ProFound AI (its workflow solution for the 2D mammography) in 2023. It should be noted that a regulatory approval process is required once product development has become completed.
“While these dates are difficult to predict and subject to change, iCAD estimates the availability of an iCAD cloud offering by the end of 2023 and the new AI solution with Google AI in the first half of 2024, depending on the time it takes to achieve regulatory clearance,” said Nicole Linton, Google’s communications manager for health artificial intelligence.
Once it’s cleared, the AI-equipped medical devices will be sold to hospitals, health systems and outpatient clinics, Stevens said. Google and iCAD did not disclose the terms of the partnership or whether they will share profits.
The partnership is also about improving access to breast imaging AI technology, Stevens pointed out. To advance this goal, iCAD will use Google Cloud’s infrastructure to deploy its technology. Using the cloud will make these tools accessible to more women, “especially women who may live in areas of the world where there are infrastructure challenges and hardware constraints,” she said.
Google selected iCAD as its partner for the first licensing of its mammography AI model because of iCAD’s “legacy of leadership” in the breast imaging AI space, according to Linton. She also said that iCAD has a well-established install base, as ProFound AI is the most widely used breast imaging AI product on the market today.
The medical device company has an install base of about 7,500 licenses of its AI technology for mammography, Stevens pointed out.
But iCAD certainly isn’t the only company selling AI technology for breast imaging. There are plenty of companies developing AI not only for mammography, but across all other imaging modalities — including Holigic, Imagion Biosystems and ViewRay.
“We’re the only vendor that offers a full portfolio of AI,” Stevens declared. “That includes breast cancer detection, automated breast density assessment, as well as being the first and still the only company to offer a short term, breast cancer risk assessment AI tool that can assess a woman’s likelihood of developing breast cancer in the next year. It has around 80% accuracy.”
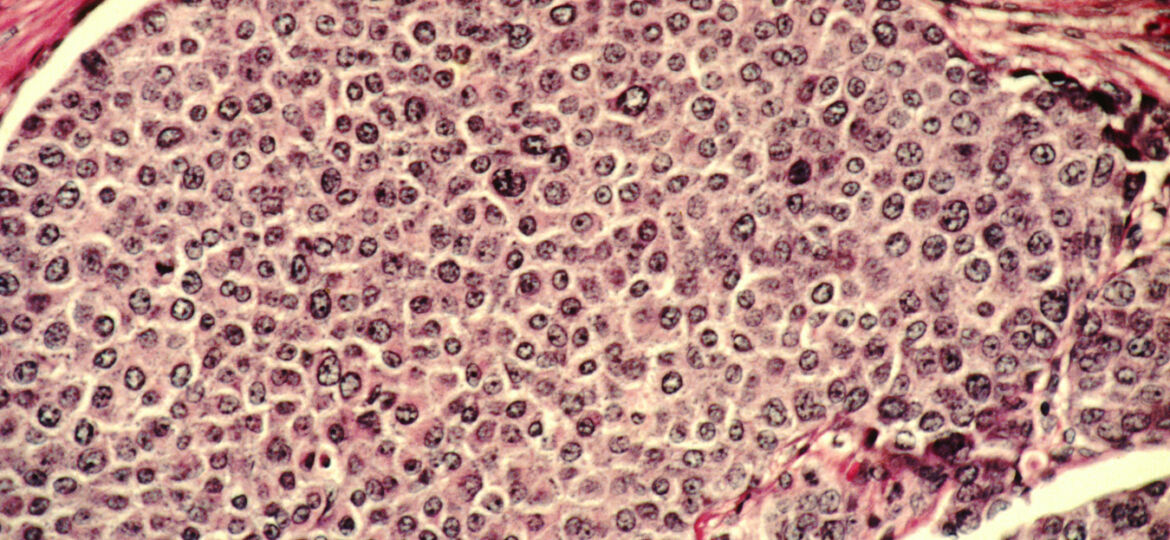
Photo: public domain image from the National Cancer Institute
Looking for a diet that can help reduce dangerous visceral fat? The Green Mediterranean diet may be the one apt for the task.The Mediterranean diet (MED) has consistently been at the top of the list of healthiest diets people can engage in. In fact, it was once again number one on U.S. News & World Report’s Best Diets this year, marking the fifth year in a row that it has taken the top spot.But when it comes to reducing visceral adipose tissue (VAT), will the traditional Mediterranean diet still come out on top? Or will the modified Green Mediterranean diet take the crown?VAT is a type of fat that’s very dangerous as it tends to wrap around one’s internal organs, the Ben-Gurion University of the Negev (BGU) noted in a news release. It has been “closely related to the development of multiple cardiovascular risk factors” and is “an independent marker of mortality,” a team of researchers noted in their study, published in BMC Medicine.
“Visceral adipose tissue (VAT) accumulation is one of the main key factors that differentiate between metabolic healthy and unhealthy obese individuals,” they wrote.Researchers looked at the impact of the Green Mediterranean diet on VAT. The Green Mediterranean diet is one that, just like the traditional one, is rich in foods like whole grains, fruits, legumes, fish and olive oil. The difference is that it is high in dietary polyphenols and green plant-based proteins, and low in red- and processed meats.In other words, it is a “greener version” of the traditional Mediterranean diet.The researchers conducted an 18-month study, the Dietary Intervention Randomized Controlled Trial PoLyphenols UnproceSsed (DIRECT-PLUS), that involved 294 participants, who followed either the simple healthy dietary guidelines, the Mediterranean diet or the Green Mediterranean diet.The participants’ adipose tissues were then examined through MRI scans. Incredibly, the team found that those who followed the Green Mediterranean diet had 14% reduced visceral fat. By comparison, those who opted for the traditional Mediterranean diet lost 7%, while those who followed the healthy diet lost an even lower 4.5% of visceral fat.This means the Green Mediterranean diet has led to a reduction in visceral fat that’s “more than twice” the VAT lost with the traditional Mediterranean diet.”A 14% reduction in visceral fat is a dramatic achievement for making simple changes to your diet and lifestyle,” said study author Hila Zelicha, of BGU. “Weight loss is an important goal only if it is accompanied by impressive results in reducing adipose tissue.”These results suggest the modified Green Mediterranean diet could be quite effective in reducing potentially dangerous visceral fat. And polyphenols might be behind the VAT loss. Polyphenols are phytochemicals present in many plant-based foods and they have been studied for their anti-inflammatory and antioxidant properties.”A green-MED diet enriched with polyphenols and decreased red meat consumption might serve as an improved version of the MED diet for targeted VAT reduction,” the researchers wrote. “Future studies are needed to explore the exact mechanisms of specific polyphenol-rich foods on visceral adiposity.”The team behind the DIRECT-PLUS trial was the first to introduce the Green Mediterranean diet, according to BGU. In a previous study, the diet was found to be even better for heart and metabolic health than the traditional Mediterranean diet.
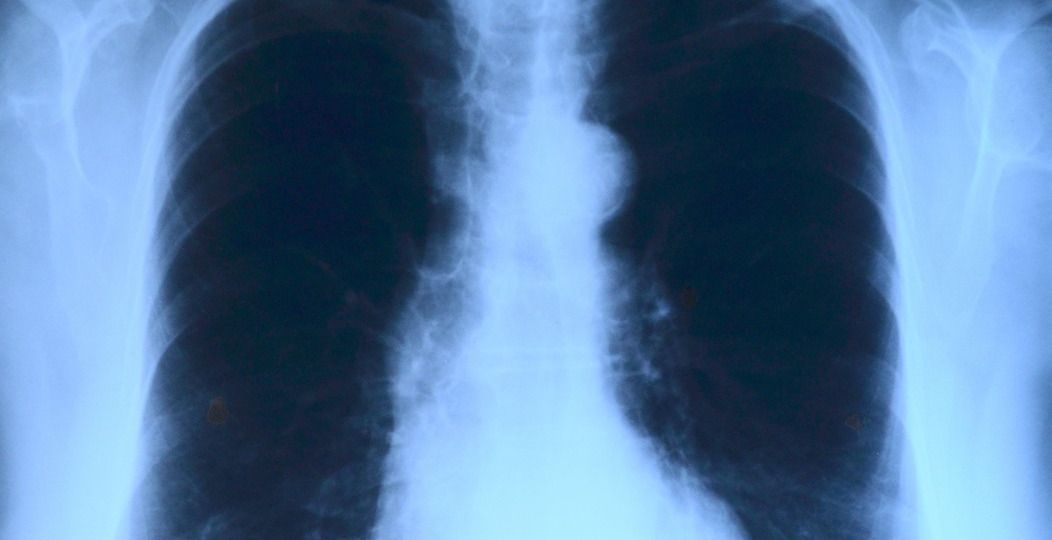
A new advanced AI can predict a 10-year risk of death resulting from atherosclerotic cardiovascular disease (ASCVD) with a single chest X-ray.The trailblazing study was presented Tuesday at the annual meeting of the Radiological Society of North America.“Our deep learning model offers a potential solution for population-based opportunistic screening of cardiovascular disease risk using existing chest X-ray images,” lead author, Jakob Weiss, a radiologist affiliated with the Cardiovascular Imaging Research Center at Massachusetts General Hospital and the AI in Medicine program at the Brigham and Women’s Hospital in Boston, said, reported SciTechDaily. “This type of screening could be used to identify individuals who would benefit from statin medication but are currently untreated.”Generally, patients at high risk of heart disease are recommended a statin drug that lowers cholesterol levels in the blood as well as protects the artery walls from within. However, it is not always easy to detect the most vulnerable people, who are missing out on the medication that could save their lives.
The deep learning model developed by the researchers can help find people who have a risk of developing heart disease within the next 10 years and bring them under the ambit of primary prevention.“We’ve long recognized that X-rays capture information beyond traditional diagnostic findings, but we haven’t used this data because we haven’t had robust reliable methods,” Dr. Weiss said. “Advances in AI are making it possible now.”Currently, doctors calculate this 10-year risk by generating a statistical model that takes into account various factors, including age, sex, race, systolic blood pressure, hypertension treatment, smoking, Type 2 diabetes, and blood tests as well as an ASCVD risk score. Patients with a 10-year risk of 7.5% or higher are advised statin medication.“The variables necessary to calculate ASCVD risk are often not available, which makes approaches for population-based screening desirable,” Dr. Weiss said, according to the outlet. “As chest X-rays are commonly available, our approach may help identify individuals at high risk.”The research team trained a deep-learning model using a single chest X-ray (CXR) input. The model, known as CXR-CVD risk, was fed 150,000 chest X-rays taken from more than 40,000 participants in a prostate, lung, colorectal, and ovarian cancer screening trial under the aegis of the National Cancer Institute.The AI was then made to predict 10-year risk in individuals from the data of more than 11,000 patients with an average age of 60. These individuals who had routine outpatient chest X-rays at Mass General Brigham were potentially eligible for statin therapy, according to ScienceFocus.It was found that 10% of the patients from this group experienced a major cardiac event within the next 10 years. The CXR-CVD Risk model succeeded in predicting 65% of the cases.“The beauty of this approach is you only need an X-ray, which is acquired millions of times a day across the world,” Dr. Weiss said. “Based on a single existing chest X-ray image, our deep learning model predicts future major adverse cardiovascular events with similar performance and incremental value to the established clinical standard.”
veryone at some point has heard of or been told about the importance of drinking at least eight glasses of water per day. A new study put this axiom to the test and found surprising results.The study, published in the journal Science, found that the quantity of daily consumption of water depends on factors such as age, gender, activity levels, and climate.”The current study clearly indicates that one size does not fit all for drinking water guidelines, and the common suggestion that we should drink eight 8-ounce glasses of water per day (~2 liters) is not backed up by objective evidence,” the researchers wrote in their paper, reported ScienceAlert.While previous studies have busted this myth, they banked on the participants to correctly report the amount of water they had consumed. This assumption that the participants will remember and disclose the exact amount of water they had leaves room for human error.
The new study relied on scientific data that detailed the amount of water consumed by the body. To give a clear answer to how much water the human body needs, the study employed more than 5,600 volunteers of different ages from 26 countries around the world.Each participant was given 100 milliliters of water enriched with 5 percent “doubly labeled water.” Doubly labeled water, safe for consumption in small amounts, has isotopes of both hydrogen and oxygen. It helps in tracking the rate of movement of chemicals through the body.”If you measure the rate a person is eliminating those stable isotopes through their urine over the course of a week, the hydrogen isotope can tell you how much water they’re replacing, and the elimination of the oxygen isotope can tell us how many calories they are burning,” the study’s co-author, Dale Schoeller from Biotechnology Center and Department of Nutritional Sciences at the University of Wisconsin explained, according to ScienceAlert.Interestingly, the University of Wisconsin–Madison lab, where Schoeller works, was the place where doubly labeled water experiments in humans were pioneered in the 1980s.”Water intake requirements largely reflect water turnover, the water used by the body each day,” researchers wrote. Hence, water turnover was the parameter used to determine the amount of water assimilated by the body.Water turnover was seen the most between ages 20 and 30 in men and women aged 20-55. Furthermore, water turnover was found to decrease beyond the age of 40 in men and after the age of 65 in women, the study found.The highest turnover of water as a percentage of all the water in the body was observed in newborns.Also, all factors being constant, men consumed about half a liter more water every day than women, according to the study.Weight also played a role in water requirement, the results showed. Every 110 pounds increase in body weight, led to an increase of 0.7 liters a day of water turnover.Meanwhile, water turnover moved up by 0.3 liters as a result of a 50% increase in humidity.The location of an individual also matters. Participants living in developed countries following a sedentary lifestyle had lower water turnover compared to participants who were manual laborers or hunter-gatherers in developing countries, the study found.”The variation means pointing to one average doesn’t tell you much,” Schoeller stated, according to the outlet.”Improved guidelines are of increasing importance because of the explosive population growth and climate change the world currently faces, which will affect the availability of water for human consumption,” the researchers concluded.
You might want to take your vitamin D levels seriously. A new study has found low vitamin D levels are associated with premature death.Researchers from the University of South Australia (UniSA ) conducted the study — published in the journal Annals Of Internal Medicine — which found the severity of vitamin D deficiency was closely linked to increased mortality risk.“While severe vitamin D deficiency is rarer in Australia than elsewhere in the world, it can still affect those who have health vulnerabilities, the elderly, and those who do not acquire enough vitamin D from healthy sun exposure and dietary sources,” first author, Josh Sutherland, and a Ph.D. student at UniSA, said, reported SciTechDaily.Vitamin D is an essential nutrient needed by the body to ensure good, healthy bones and muscles.
“Our study provides strong evidence for the connection between low levels of vitamin D and mortality, and this is the first study of its kind to also include respiratory disease-related mortality as an outcome,” Sutherland continued. “We used a new genetic method to explore and affirm the non-linear relationships that we’ve seen in observational settings, and through this, we’ve been able to give strong evidence for the connection between low vitamin D status and premature death.” Speaking of challenges in conducting efficient studies on the relation between vitamin D and death risk, Sutherland said, “Vitamin D deficiency has been connected with mortality, but as clinical trials have often failed to recruit people with low vitamin D levels – or have been prohibited from including vitamin deficient participants – it’s been challenging to establish causal relationships.”For the study, the researchers scrutinized 307,601 records from the UK Biobank, which has participants recruited between March 2006 and July 2010.Vitamin D levels less than 25 nmol/L were considered low. The average vitamin D concentration was found to be 45.2 nmol/L.Senior investigator and Director of UniSA’s Australian Centre for Precision Health, Professor Elina Hyppönen, said more research will help inform public health strategies, which, in turn, will help formulate national guidelines.“The take-home message here is simple – the key is in the prevention. It is not good enough to think about vitamin D deficiency when already facing life-challenging situations when early action could make all the difference,” Hyppönen said. “It is very important to continue public health efforts to ensure the vulnerable and elderly maintain sufficient vitamin D levels throughout the year.”Another vitamin, B3, is in the news. A study has found the vitamin B3 supplement nicotinamide riboside (NR), promoted as an anti-aging product, may increase cancer risk and brain metastasis.”Some people take them [vitamins and supplements] because they automatically assume that vitamins and supplements only have positive health benefits, but very little is known about how they actually work,” co-author Elena Goun explained. “Because of this lack of knowledge, we were inspired to study the basic questions surrounding how vitamins and supplements work in the body.”
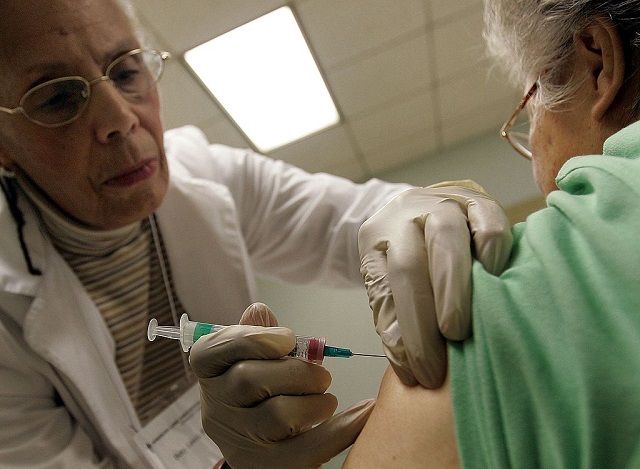
As the U.S. enters the holiday season, there is fear that the flu situation could get more alarming in the coming weeks. Based on the latest data from the Health and Human Services Department, flu hospitalizations have increased by nearly 30% in a week. More than 11,200 people were hospitalized due to the flu virus in the week ending Nov. 19, CNBC reported Monday. Compared to the previous week which recorded about 8,700 hospitalizations, there’s been a big jump in cases, leading experts to believe that the spread of the respiratory illness has remained high across the country. Flu season started earlier than usual this year, taking a toll on the emergency departments and hospitals amid the ongoing COVID-19 pandemic. In the past, flu activity typically picked up after Thanksgiving. But hospitalizations were already significantly high in early November this time around.
“The fact that we’re already at this high level going into the holiday season makes me nervous,” microbiologist and flu expert at the Penn Institute for Immunology Scott Hensley told the outlet. As early as October, flu activity in the country already set a record. About 11 people out of 100,000 have been hospitalized, the highest level recorded in a decade. According to the Centers for Disease Control and Prevention (CDC), around 35 states have been experiencing high or very high flu activity. Only 6 states were reporting low activity, and most were in the north. This flu season alone, more than 6.2 million people have fallen ill due to the influenza viruses, around 53,000 have been hospitalized, and 2,900 have reportedly died. As flu activity continues to climb higher, public health experts worry that more pediatric deaths could be reported in the coming weeks. Just recently, five more pediatric cases reportedly died, bringing the season’s total to 12, said the Center for Infectious Disease Research and Policy. The pediatric deaths reportedly occurred between early October and mid-November. All of the cases involved influenza A. H1Na and H3N2 were the two subtypes reported among the pediatric deaths. Though vaccine efficacy data has not been published yet, experts said they worked well with the newer strains. Hence, they encouraged everyone to get vaccinated to stay protected for the remainder of the flu season. “From what we can see, it looks like the vaccines are pretty darn good matches to what’s circulating. If there’s ever a time to get vaccinated, this is the year to do it,” Hensley said.